Maybe you noticed a bump down there. Or an itch. Or a funky smell. Or burning after you pee. But something’s for sure: something’s not right down there. Or in the more common scenario, maybe you didn’t notice anything at all! If you’ve ever had a run-in with a sexually transmitted infection, you’re not alone.
Because here’s the facts, Betties: 1 in 5 people in the U.S. have had a sexually transmitted infection (STI). *oof*
What that stat tells us: STIs are realllllllly common! But they don’t have to be.
The tricky thing about STIs is many infected don’t have noticeable symptoms, and as a result, never test, and often unknowingly become spreaders. *sigh* Betties, STIs disrupt your sexual health – physical, emotional, mental and social well-being – and because Betty’s advocates for the health of your whole self, we need to have a serious, stigma-free chat about STIs.
So tell me this, how exactly are STIs transmitted?
A person with an STI can pass it to another person through skin, genital, mouth, rectum, or bodily fluid contact.
A common misconception is STIs are exclusively spread through penetrative sex.
However, depending on the infection, STIs can be spread in different ways:
– Digital, vaginal, oral or anal sex
– Contact with blood & blood products or body fluid
– Needles (accidental stick or sharing)
– Skin to skin or kissing
– Some can be passed from mother to child during pregnancy and childbirth
How long does it take for STI symptoms to appear?
The time it takes for an infection to develop after a person has been exposed to a disease-causing organism (AKA when they might see symptoms) is called the incubation period. The STI contracted will dictate when you might begin to experience symptoms:
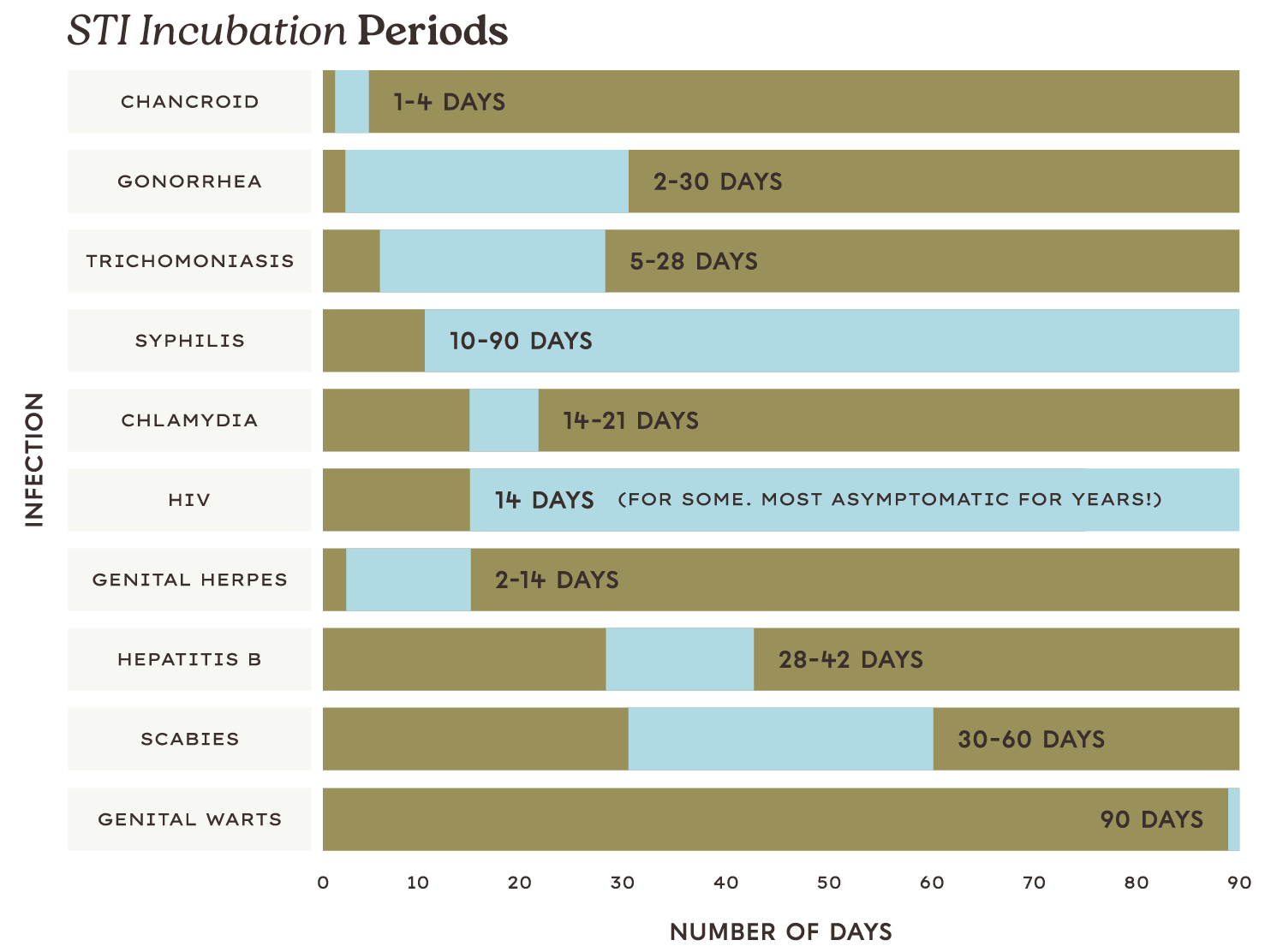
It’s important to note, if you test for an STI too early and the incubation period is not over yet, you may test negative for the disease even if you do have it.
Who is at the highest risk for STIs?
Betties run the risk of becoming infected if they:
– Have or have had more than one sexual partner
– Have or have had a partner with more than one sexual partner
– Have vaginal, oral, or anal interaction with someone who has an STI
– Have a personal history of an STI
– Used to have or have a partner(s) who use intravenous drugs (drugs injected into a vein)
– Have a weak immune system
So are STIs basically all the same?
Nope! STIs fall into three major categories:
1
BACTERIAL INFECTIONS
2
viral INFECTIONS
3
parasitic INFECTIONS
By learning some STI differentials, you’re already a step ahead in prevention practices! Now let’s get into the particulars of some of the most common STIs.
BACTERIAL INFECTIONS
What is it?
Gonorrhea and chlamydia are two of the most commonly reported STIs in the United States. Gonorrhea and chlamydia are each caused by a different type of bacteria and often occur together.
How can I tell if I have it?
The truth is, you may not be able to tell for sure! Those infected are often asymptomatic, but those with symptoms experience pelvic pain and/or discharge. Left untreated, both can cause long-term pelvic pain and infertility.
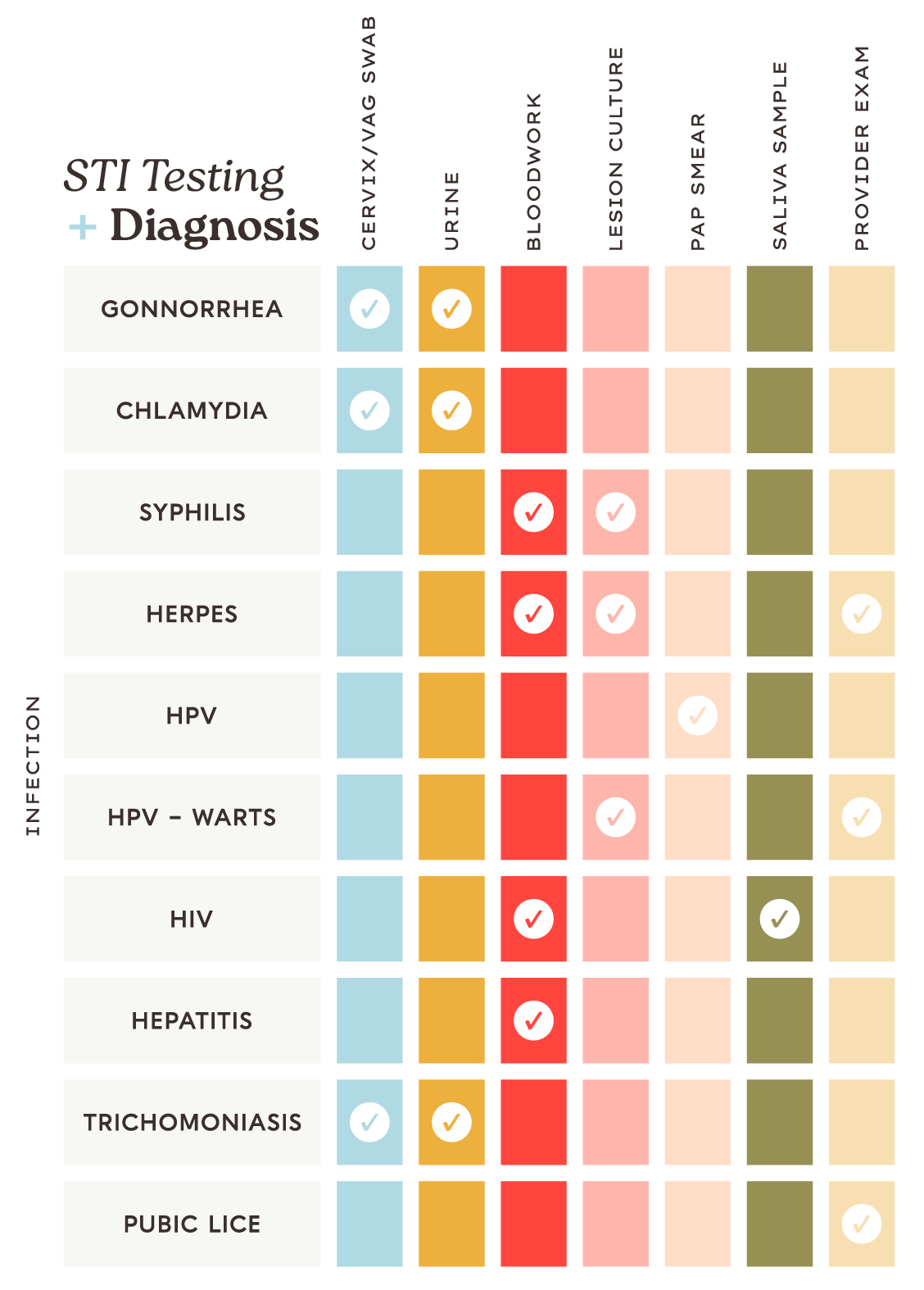
How is it diagnosed + treated?
Both infections can be diagnosed through a urine test or cervical swab and treated with antibiotics.
What is it?
Syphilis can be transmitted through direct or indirect contact with lesions or bodily tissues.
How can I tell if I have it?
Like many STIs, you might not initially notice if you’ve contracted syphilis. Syphilis is a bit unique in that it develops in three stages:
STAGE 1: Syphilis first appears as a painless, round sore on the genitals.
STAGE 2: If not treated, syphilis progresses to mild, flu-like symptoms
STAGE 3: The last stage is later in the disease development and can cause severe health issues in all the organs of the body.
How is it diagnosed + treated?
A healthcare provider will most likely use a blood test to diagnose syphilis but can also test the fluid from a syphilis sore to make a diagnosis. Depending on the stage, syphilis can be treated with antibiotics. Betties, if you feel you may have been exposed, you know the drill: get tested!
PARASITIC INFECTIONS
What is it?
Trichomoniasis (“Trich”) and pubic lice (AKA “crabs”, which has nothing to do with those creepy crawlers on the beach ;)) are both parasitic infections. While trichomoniasis is transmitted through sexual intercourse, pubic lice can be additionally spread through sharing clothes, towels and/or beds.
How can I tell if I have it?
Trich: For vagina-havers, trichomoniasis can cause frothy discharge of varying colors: greenish, brownish, grey or white. Other symptoms can include a fishy odor and itching.
Pubic Lice: Like head lice, extreme itching near your genitals can be a dead giveaway for pubic lice.
How is it diagnosed + treated?
Both can be diagnosed from a pelvic swab exam and can be treated with medication.
Anything else I should know?
Shaving does not get rid of pubic lice, so put down that razor and get tested!
VIRAL INFECTIONS
What is it?
HPV, is the most common STI in the United States. Certain types of HPV can cause abnormal changes in the cervix that may lead to cervical cancer. With more than 200 strains, it’s also linked to cancer of the anus, vulva, vagina, penis, head, and neck.
How can I tell if I have it?
Generally, those infected experience no symptoms, but a few types can cause genital warts.
How is it diagnosed?
HPV can be detected through screening tests and a Pap smear.
How is it treated?
The bad news: HPV has no cure. Most infections can be cleared on their own, but not all. Some can progress to cancer. The good news: A vaccine is available to prevent several of the most dangerous types of HPV! This vaccine is available for anyone 9 years and older. Haven’t been vaccinated? Consult your provider to see whether you need the HPV vaccine!
What is it?
HIV is transmitted through contact with infected body fluids (e.g. semen, vaginal fluid or blood). This virus depletes the immune system by attacking the body’s T-cells (whose job is to fight infection). Left untreated, HIV can cause AIDs (Acquired Immunodeficiency Syndrome).
How can I tell if I have it?
Unless you are tested, you may not know you have HIV until you get sick. Some will have flu-like symptoms within 2-4 weeks after becoming infected.
How is it diagnosed?
An HIV diagnosis can only be made through a saliva or blood test.
How is it treated?
Unfortunately, HIV is not curable, but medication can help control the virus.
HIV prevention is also supported by taking PrEP(pre-exposure prophylaxis), a daily pill that can reduce risk by blocking the pathways HIV uses to set up the infection and can prevent its spreading. If you have questions or want to see if you’re a good candidate for PrEP, make a Care appointment to talk with one of our providers.
What is it?
Herpes belongs to a family of viruses. Two of its strains (or types) result in oral herpes and genital herpes. Herpes can be transmitted through oral, anal or vaginal sex or via contact with a herpes sore.

Herpes is predicted to affect almost 67% of the world having oral herpes and 12% have genital herpes.
How can I tell if I have it?
Herpes is tricky because it may be mistaken for a pimple or an ingrown hair. So here’s what to look for: Herpes will appear as a single sore or cluster of sores on/around a mucous membrane such as the mouth, genitals or rectum. These’ll often burn, itch or tingle. An outbreak- especially a first-time outbreak can also include flu-like symptoms such as headache and fever.
How is it diagnosed?
If you’re exposed, hit up your medical provider to make a diagnosis via bloodwork or a culture sample of a sore.
How is it treated?
Unfortunately, herpes is a chronic virus that will make recurring appearances. But herpes outbreaks can be managed through medication and, for those with frequent outbreaks, suppressive therapy can help reduce outbreaks by 70-80 percent.
How can I prevent getting or giving an STI?
Betties, 15-24-year-olds account for half of all new infections, and that means we can make an impact in reducing the transmission rate. STIs might be common, but they still have a lot of stigmas in need of squashing through awareness and education. The more we know, the less we spread. And the more we talk openly about STIs, the more we normalize practicing prevention and getting tested!
If you’re experiencing symptoms, have questions about STIs or just want to get a check-up, make an appointment with Betty’s Co.We’re here to support your sexual health as a stigma-free space for you to test + talk with our providers about treatment and prevention.







Join the conversation